Overview
Pneumonia Community Case Management (CCM)
The WHO Integrated Management of Childhood Illnesses (IMCI) guidelines prescribe how children under 5 should be managed at primary health care facilities. For the diagnosis of pneumonia, health facility staff workers should assess whether a child has fast breathing by measuring their respiratory rate. For children between 2-12 months, a diagnosis of pneumonia is determined when they present with 50 or more breaths per minute. For children from 12 months to 5 years the threshold is 40 breaths per minute.
Studies show that community health workers (CHWs) can also be trained to manage pneumonia cases according to the IMCI guidelines. They are highly motivated individuals who live in the community where they work. After receiving specialized training, usually by the Ministry of Health, they provide care and treatment for children beyond health facilities. Often in these settings there is no electricity, running water or motorized transportation.
There is accumulating evidence that with appropriate supervision, CHWs can make a significant impact in reducing child mortality. Large scale community case management (CCM) pneumonia programmes are currently running in several countries, including Pakistan, Ghana, Uganda, Ethiopia and Rwanda.
In addition, CHWs providing home-based newborn care are now also being trained to identify fast breathing during their home visits after birth.
Acute Respiratory Infection Timer
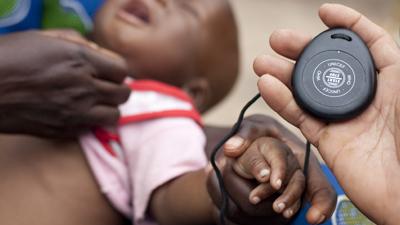
To help health workers determine how long they need to count a child’s breaths, UNICEF and WHO developed a one-minute Acute Respiratory Infection (ARI) Timer in the 1990s. In the last five years nearly half a million timers have been supplied to over 70 countries. In line with the increasing adoption by Ministries of Health of pneumonia CCM policies, UNICEF procurement for it increased from 25000 in 2005 to 122000 in 2010.
However, anecdotal feedback from pneumonia CCM experts indicated the need to re-design the ARI Timer. Subsequent user research (see Resources) in Ghana and Uganda has given CHWs an opportunity to co-create an improved diagnostic tool. The research confirmed that the ticking sound it makes, to indicate to the CHW that the timer is functioning, distracts during the count. The alarm at 30 seconds is startling to the parents and can confuse the CHW whether the end of the minute has been reached or not. Improvements are currently being implemented through a new product specification to ensure that future ARI Timers will be more fit for purpose.
Determining Breath Rates
In addition to monitoring the one-minute time requirement, the CHW also needs to assess the breath counts. These can go up to as high as 60-70 breaths per minute. Focusing on a child for a full minute, while visually identifying breaths and counting silently is more difficult than it first appears. The child may become restless, the CHW may not be able to concentrate and simply lose track. CHWs also worry that they do not see all the breaths. This potentially leads to recounts, time lost and reduced accuracy.
CHWs who are not numerically literate have difficulties with counting and working with numbers. Counting breaths and applying against prescribed age-specific IMNCI thresholds can be difficult to determine by them.
Simplifying Countings
Solutions are being explored to help CHWs keep accurate count. In Ghana, Uganda and South Sudan, Save the Children, International Rescue Committee and UNICEF have piloted and implemented the use of counting beads. Similar to prayer beads, counting beads is a concept that already exists in many communities.
Pilot tests show that a combination of color-coded and age-specific strands of beads can greatly improve the accuracy of pneumonia diagnosis. The impact is most significant in remote areas where CHWs may have had less schooling and fewer opportunities to learn about numbers and counting. The age-specific colour-coded strands remove the need to interpret the breath count against the cut-off rates. The color-coding is also a tool to communicate the diagnosis. A parent, who can “see” the diagnosis expressed in beads, is less likely to insist on antibiotics if that type of treatment is not necessary – and potentially harmful.
Based on these initial findings and potential diagnosis improvements UNICEF Supply Division is currently considering the development of an “ARI counting beads” design guide. It would instruct how to assemble ARI counting beads so that count accuracy will be improved, while using locally-procured materials.
High Trust in Technology
The user research also showed that patients do have some experience with ‘low-tech’ health products, such as thermometers, stethoscopes, blood pressure meters and pregnancy tests, and they have a high degree of trust in them. Patients generally believe that health technology reduces human error. When one of these tools is used on them, people feel that they have been properly examined; raising confidence in the health worker and potentially reducing their desire to self-medicate, use traditional healing methods or seek advice from unlicensed ‘chemists’.
Creating the Dream Solution: ‘the Judge’
Despite a redesign of the ARI Timer and ARI counting beads, the ideal solution would be a device that could automatically detect pneumonia. Such an automated tool would be relevant for both (primary) clinics, where there is a higher patient load, and to improve the quality of care given by CHWs.
As a CHW in Uganda put it: “…We need a Judge to decide if the child should receive treatment or not and to also tell this to the mother…”. For many CHWs participating in user research on pneumonia diagnostics, an ideal device is something that can be put on the child, somehow does the counting and diagnosis on its own and then shows the result in a way that the child’s mother would understand. This would also help to reduce “wasting drugs” on children that just have a common cough or cold.
The device would also be durable enough to withstand extreme environmental conditions and not reliant on electricity or other power source that is unavailable in many settings. For patients and families a clean but sophisticated look and feel would add to its credibility.
While there are developments on the horizon, appropriate rapid diagnostic tests for point of care application are not available on the market at the moment. Based on existing technologies UNICEF is advocating for the development of a tool that could automatically and precisely determine respiratory rates in children under 5.
A target product profile is currently being developed and will be posted on this site. In the meantime, please see the resources page for more detailed background, documents, web links and user research reports.
Knowledge Sharing
If you, your organization or company are working on or aware of an innovative solution for childhood pneumonia diagnosis in low-resource settings then please get in touch with us through the Get Involved page. Further related information can be found under Resources.
Get Involved
Please do get in touch with us if you would like to share:
- Feedback from current ARI timer and counting beads usage
- Examples of other tools currently being used to support pneumonia diagnosis
- Relevant products and technology that are under development. Please also see our Request for Information
- Other ways you would like to support this project
To get involved click here